It was the weekend and I thought the pain would probably be gone by the next day. But come Monday it was still there and as the week went on it got worse.
My left leg started to feel numb and by the end of Tuesday I was practically dragging my leg around. I thought it must be a pinched nerve. Instead of kicking off my shoes and grabbing a cool drink with friends after work, I couldn’t wait to strip my jeans from my now swollen leg. My mom massaged my thigh every night and I kept thinking it would get better. After all, I was 22, active and healthy. But on Saturday morning I woke up in excruciating pain.
My left leg wasn’t only swollen, it had turned purple. I was unable to drive so my mom took me to our doctor where we finally discovered what was wrong – it was a blood clot. I needed blood-thinning tablets and two days’ bed rest, I thought. But it wasn’t as simple as that.
Instead I was rushed to hospital and admitted. Only then did I realise how serious it was. I was diagnosed with deep vein thrombosis (DVT) and ended up spending the next week in hospital. I had to lay still because moving around could dislodge the clot.
I was given medication every 12 hours, my blood was drawn to be tested three times a day and an ultrasound scan was done to establish exactly where the clot was – in my left groin. Further tests revealed I have a genetic blood-clotting condition. Being on the contraceptive pill had increased my risk of a blood clot.
After a few weeks of bed rest – my leg was so swollen, stiff and painful I couldn’t bend or move it – followed by a few weeks on crutches, I slowly started walking unaided again. I’ll have to take blood thinners daily for the rest of my life because the DVT is partly due to my genetic condition.
I’d started taking the Pill last year and had no idea there was a risk of blood clots. About a month later I donated blood and this time it took longer because my blood was thicker. It was a warning sign, but because the nurse couldn’t find anything “wrong” with me I didn’t think anything of it.
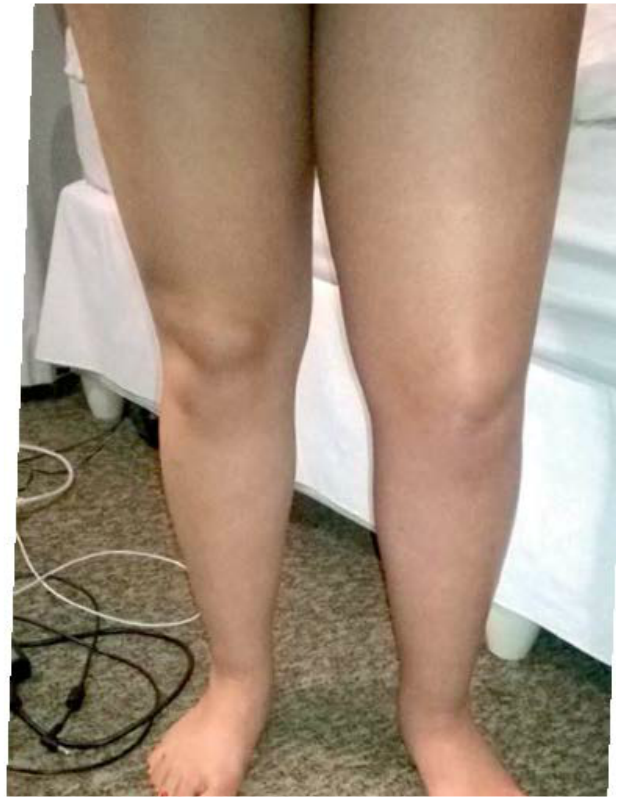
After my mom rushed me to the doctor that day, his first question was, “Do you use a contraceptive pill?” At the hospital the nurse and doctors asked me the same question. Why hadn’t anyone warned me about this? It happened five months ago and today I still have one leg that fits into size 32 jeans while the other fits more comfortably into size 34.
I still have the clot – it will be surgically removed in October as I’ve joined a new medical aid and there’s a waiting period. The procedure also involves having a stent inserted.
READ MORE: Could your birth control give you deep vein thrombosis?
WHAT IS DVT?
There are two sets of veins in your legs that return blood to the heart and lungs: the smaller, superficial veins you can see under your skin, and the bigger ones deep in your muscles. Deep vein thrombosis, as the name suggests, is a blood clot that forms inside a deep vein.
DVT most often occurs in the calf, but can also form in the groin or abdomen, which is more serious.
In women, blood clots are more common in the left calf, Dr Judith Kluge of Stellenbosch University’s gynaecology and obstetrics clinic at Tygerberg Hospital in Cape Town, says.
WHAT ARE THE SYMPTOMS?
Half the people who develop DVT have no warning signs. Those who do can experience one or any combination of the following:
- Leg pain (similar to a pulled muscle)
- Swelling
- Redness of the skin of the calf/leg
- Skin that feels hot
- Discolouration of the skin
- A feeling of tiredness in the leg
HOW DANGEROUS IS IT?
DVT can be dangerous as the clot, or part of it, can break off and travel through your bloodstream. “It can then travel up through the heart and end up in the lungs where it can block blood flow, causing organ damage or death,” explains Dr Pieter Zwanepoel, a vascular surgeon at Milnerton Mediclinic in Cape Town.
“This is referred to as pulmonary embolism (PE) and it can either be asymptomatic or it can be fatal,” he says. There’s also the danger of complications at a later stage, including enlarged veins, chronic tiredness of the legs and swelling.
Severe cases of DVT can lead to post thrombotic syndrome (PTS). This is when the blood clot damages the vein and affects blood flow. It can lead to higher blood pressure in the leg, which can cause swelling, skin pigmentation and ulcers.
The first symptoms of PTS could surface only three to five years after the DVT. Statistics aren’t available for South Africa, but globally about one in 1 000 people a year develop DVT.
HOW IS IT TREATED?
Anticoagulants (blood thinners) are ingested in pill form or by injection. Although they’re known as blood thinners they don’t actually thin the blood – they make it less “sticky” to stop the clot getting bigger and prevent new clots from forming.
The medication doesn’t break up the clot – your body’s enzymes do that and it can take between one and three months. The blood thinners simply give your body time to dissolve the clot on its own. Treatment lasts for at least three months. When the clot is in the groin or higher up, surgery is usually advised to remove it.
WHAT CAUSES DVT?
“Blood wants to flow inside a nice smooth vessel,” Dr Zwanepoel says. “Anything that interferes with the blood, the flow or the vessel can lead to the formation of DVT.” Blood that’s thick or flows slowly is more likely to form a clot, especially in a vein that’s already damaged. You’re at higher risk of DVT if you:
- Are on extended bed rest
- Have cancer
- Have had surgery
- Are older
- Smoke
- Are overweight or obese
- Sit for an extended period, such as on a long flight
- Use medication that increases blood clotting, such as the contraceptive pill
- Have an underlying genetic clotting disorder
- Have enlarged veins
- Have had DVT before
“Many people walk around with a genetic blood disorder without developing DVT,” Dr Zwanepoel says. “But one additional small risk factor, such as a long flight or taking the Pill, can tip the scale just enough for them to develop DVT.” About one in every 30 people who’ve had DVT will develop it again, he adds.
Women are also more likely to develop DVT during pregnancy and in the four to six weeks after giving birth, as the higher levels of oestrogen in the body can make blood clot more easily. The pressure of a pregnant woman’s expanding uterus can also slow blood flow in the veins.
Birth control pills raise the amount of the hormone oestrogen in the blood, increasing the risk of DVT.
The artificial oestrogen used in most contraceptives is potent and stimulates the liver, resulting in greater clotting than with natural oestrogen, says Dr Judith Kluge of Stellenbosch University’s gynaecology and obstetrics clinic at Tygerberg Hospital in Cape Town.
Some things to keep in mind if you’re on contraceptives:
Today’s contraceptive pills contain just a fraction of the oestrogen used in the first contraceptive pill developed in the ’60s. Pills that use oestrogen in combination with the hormone progesterone have less of a clotting risk than oestrogen-only pills.
The pills developed in the ’70s, such as Nordette and Oralcon, have the lowest clotting risk. Pills developed more recently, such as Yaz and Yasmin, have a slightly higher clotting risk but are often prescribed because they help to reduce acne and premenstrual tension symptoms. “But the risk of DVT, regardless of which Pill you use, is actually very low in healthy young women,” she says. “I often say it’s not so much about the contraceptive being risky, but rather the woman herself.”